Intro
This blog marks the beginning of a concept for me as I look to expand on previous bits of work I have completed. For example I wrote an article for PhysioFirst which you can read in full here. It has topped 9000 downloads at the time of writing this blog and I am immensely proud of it as a piece of work, it was however hamstrung by a word limit and primarily about the joint dysfunction component of RA. This forced me to leave important components out of the document, you can understand them not wanting me to submit a book length article to them but for me it left a lot of things unsaid that I feel would be helpful to Physios. As a result I will look at expanding on these concepts and adding fresh ones.
As usual feedback is gratefully received as are any materials I might be interested in!
PLEASE REMEMBER – THIS BLOG IS NOT A REPLACEMENT FOR CLINICAL REASONING, IF YOU ARE UNSURE GET ADVICE
Overview and Characteristics of Rheumatoid Arthritis
“Rheumatoid arthritis (RA) is a chronic inflammatory disease characterised by joint swelling, joint tenderness, and destruction of synovial joints, leading to severe disability and premature mortality” (Alehata et al 2010). It is of interest to Physiotherapists as guidance recommends therapies which offer areas of expertise in exercise and education regarding the condition and general health (Luqmani et al 2006, Luqmani et al 2009). The persistent synovitis of the joints presents as swelling, heat, stiffness and pain that is usually worse in the early part of the day. The presence of inflammatory infiltrate, if left untreated by medication, eventually causes irreparable erosion to the joint structure which can be extremely disabling. While the Metacarpophalangeal Joints (MCPJs) are the most commonly affected, any synovial joint can be affected and large joint replacements occur at a younger age in RA sufferers (Lee & Choi 2012).
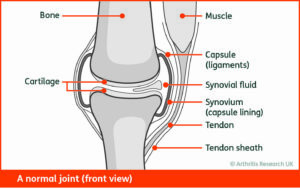
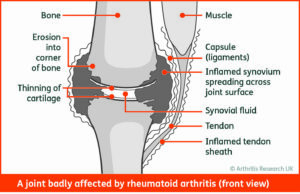
Thanks to ARUK (now versus arthritis) for their kind permission to use these images
Traditionally sufferers of RA have required large amounts of input from different specialisms such as Rheumatologists, Orthopaedic Surgeons and Therapists however improvements in early detection and management from a medical point of view has significantly improved patient outcomes and prolonged function (Stoffer et al 2016). This improvement in medical management has led to the requirement to change Physiotherapy approach, no longer is it consistent of splinting, wax bath treatment and hydrotherapy but more exercise and education on self-management of the condition to return/maintain high level function.
Rheumatoid Arthritis is an extremely variable condition in almost all its characteristics. Symptom severity, number of joints affected, associated symptoms such as fatigue or malaise and age of onset are all individual in their presentation. In addition to the variability of the condition the person themselves brings with them their own beliefs, tolerances, requirements and functional challenges.
In addition to the obvious impact on joints, RA has multisystem affects causing heightened risk of Cardiovascular Disease, Osteoporotic fractures, incidence of infection and development of some malignancies (Giles 2015).
Check out some more of my Rheumatoid Arthritis work https://chewshealth.co.uk/download/suspect-rheum/ and https://rheumatology.physio/pregnancy-and-rheumatoid-arthritis/
There is also a lecture from me on Trust Me Ed, sign up, it is super worth it!
Sign up for the rheumatology.physio newsletter HERE
References
Alehata D, Neogi T, Sliman A, Funovits J, Felson D, Bingham C, Birnbaum N, Burmester G, Bykerk V, Cohen M, Combe B, Costenbader K, Dougados M, Emery P, Ferraccioli G, Hazes J, Hobbs K, Huizainga T, Kavanaugh A, Kay J, Kvien T, Laing T, Mease P, Menard H, Moreland L, Naden R, Pincus T, Smolen J, Stanislawska-Biernat E, Symmons D, Tak P, Upchurch K, Vencovsky J, Wolfe F, Hawker G. 2010 Rheumatoid Arthritis Classification Criteria. Arthritis and Rheumatism 2010:62(9):2569-2581
Giles J. Cardiovascular Disease In Rheumatoid Arthritis: Current Perspectives on Assessing and Mitigating Risk in Clinical Practice. Best Practice & Research Clinical Rheumatology 2015:1-15
Luqmani R, Hennell S, Estrach C, Birrall F, Bosworth A, Davenport G, Fokke C, Goodson N, Jeffreson P, Lamb E, Mohammed R, Oliver S, Stableford Z, Walsh D, Wasbrook C, Webb F. British Society for Rheumatology and British Health Professionals in Rheumatology Guideline for the management of Rheumatoid Arthritis (The first 2 years). Rheumatology 2006:45(9):1167-9
Luqmani R, Hennell S, Estrach C, Basher D, Birrell F, Bosworth A, Burke F, Callaghan C, Candal-Couto J, Fokke C, Goodson N, Homer D, Jackman J, Jeffreson P, Oliver S, Reed M, Sanz L, Stableford Z, Taylor P, Todd N, Warburton L, Washbrook C, Wilkonson M. British Society for Rheumatology and British Health Professionals in Rheumatology Guideline for the management of Rheumatoid Arthritis (after the first 2 years). Rheumatology 2009:48(4):436-9
Lee J, Choi C. Total Knee Arthroplasty in Rheumatoid Arthritis. Knee Surgery and Related Research 2012:24(1):1-6
Stoffer M, Schoels M, Smolen J, Aletaha D, Breedveld F, Burmester G, Bykerk V, Dougados M, Emery P, Haraoui B, Gomez-Reino J, Kvien T, Nash P, Navarro-Compan V, Scholte-Voshaar M, Vollenhoven R, van der Heijde D, Stamm T. Evidence for Treating Rheumatoid Arthritis to Target: Results of a Systematic Literature Search Update. Annals of the Rheumatic Diseases 2016;75:16–22.


